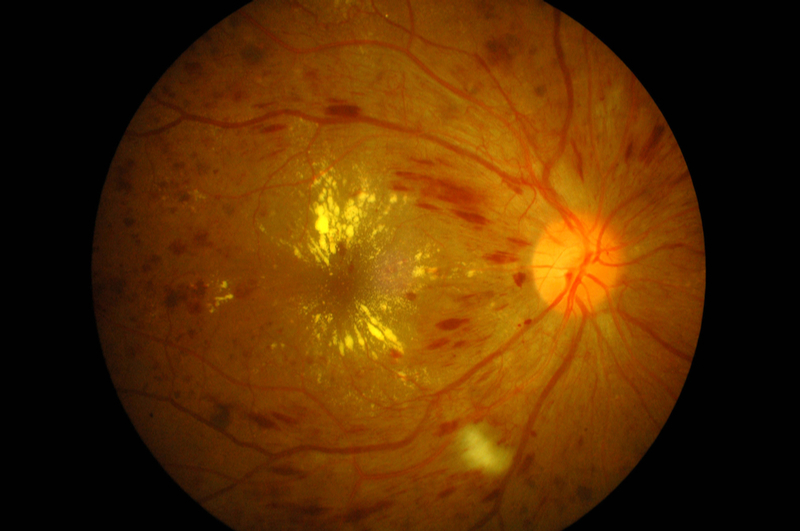
Patients with diabetes develop ophthalmic complications and especially changes in the retina.
Half of patients with Diabetes type I develop diabetic retinopathy changes in 10-15 years from their diagnosis.
Factors that contribute to development and progression of diabetic retinopathy include poor diabetes control, hypertension, hyperlipidaemia and smoking.
Diabetic retinopathy is classified into non proliferative type and proliferative type. Non proliferative changes include microvascular anomalies, retinal exudates, haemorrhages and macular edema. Proliferative retinopathy is characterized by growth of new abnormal vessels that can cause haemorrhages and retinal detachment in advanced cases. The most common cause of vision loss in patients with diabetic retinopathy is macular edema.
Proper diabetes and blood pressure control is imperative for prognosis improvement. Macular edema is treated with monthly anti-VEGF injections. Steroid injections are used as an alternative for patients that do not respond well to anti-VEGF treatment. Ischemic areas of the retina are treated with laser treatment in order to prevent further damage such as hemorrhage or retinal detachment. Tractional retinal detachment is treated with vitrectomy and fill of the vitreous cavity with silicone oil.