Frequent questions and information about Blepharoptosis.
What are the causes of ptosis?
Ptosis can be either congenital or acquired. Congenital ptosis occurs when the child is born with a defect in the levator muscle that lifts the eyelid. This can occasionally affect the visual development if it blocks part of the visual field and needs urgent surgical repair. Acquired ptosis is most commonly age-related, where the levator muscle gets stretched and does not fully lift the eyelid up. Other rare causes of acquired ptosis include neuromuscular disorders, chronic contact lens wear, eyelid tumours, injuries or previous eye surgeries.
A patient should urgently seek an ophthalmologist in case of a sudden onset ptosis accompanied by double vision, headache and eye movement restriction as a severe neurological disorder could be present.
What are the symptoms of ptosis?
Ptosis can cause a significant cosmetic issue to the patient. In more advanced cases it can affect the vision and the visual field. Ptosis can lead to severe headaches due to the constant strain to compensate for the droopy eyelid by lifting the brows.
How is ptosis diagnosed?
The diagnosis is most commonly based on clinical examination only. Blood tests are rarely required such as in cases of suspicion of underlying neuromuscular disorders ( Myasthenia Gravis).
How is ptosis treated?
Ptosis treatment is surgical and includes reattaching the levator muscle to the tarsus, which is the supporting structure of the eyelid. The surgery is performed under local anesthesia and takes around up to 30-45 minutes. Sutures are occasionally needed and if used, they are removed one week after the surgery. Congenital ptosis is corrected with frontalis suspension, a procedure where a non-absorbable suture is used to connect the frontalis muscle of the forehead to the eyelid.
Before the surgery
A detailed medical history will be taken and any blood thinning medication will need to be stopped prior to surgery; the timeframe here depends on the type of medications used. Any non-steroidal anti-inflammatory drugs should be stopped 10 to 14 days prior to surgery as they also increase the intraoperative bleeding risk.
Postoperative care
A pressure dressing is used for one day and then antibiotic and anti-inflammatory drops are applied for 2 weeks. Return to work is possible one week after the procedure.
Photos before and after
Bilateral ptosis correction

Bilateral ptosis correction 1 hour.

Bilateral ptosis correction one week.

Bilateral ptosis correction postoperatively.

Before bilateral ptosis correction combined with upper lid blepharoplasty.

Straight after bilateral ptosis correction combined with upper lid blepharoplasty.

Before bilateral ptosis correction without external incision.
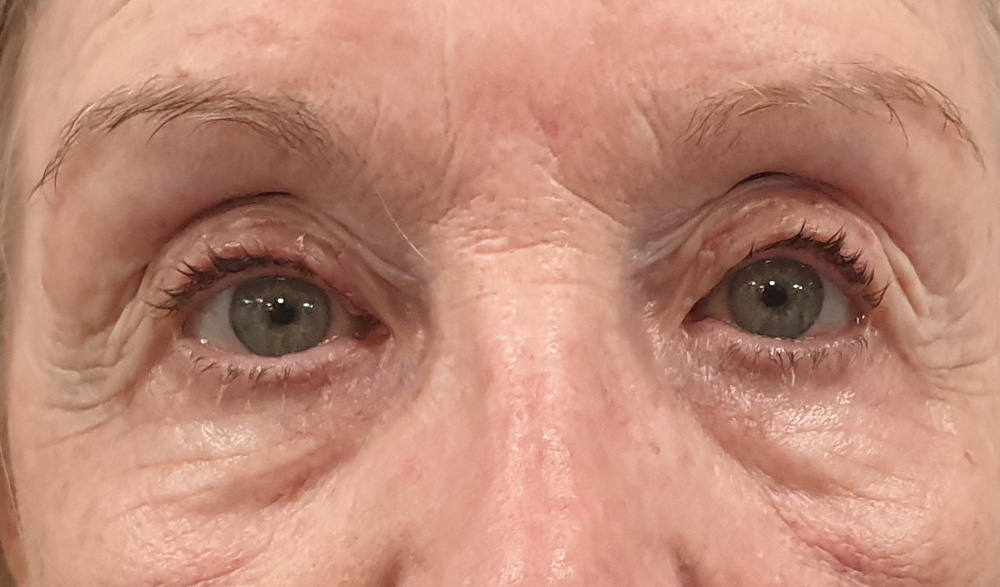
One week following bilateral ptosis correction without external incision.

Before correction of right upper lid congenital blepharoptosis in an 8-year old girl.
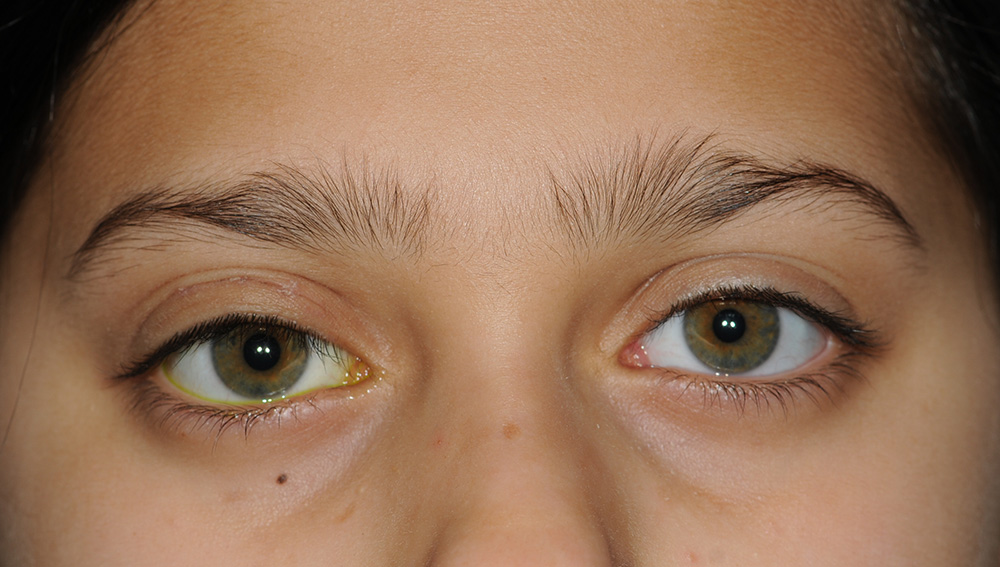
One month following correction of right upper lid congenital blepharoptosis in an 8-year old girl.


Bilateral upper lid ptosis correction in a patient with known Myasthenia Gravis via the anterior approach. Satisfactory outcomes can be achieved even in this challenging group of patients aiming at initial undercorrection.


Before and 1 week following left upper lid ptosis correction via the posterior approach.